Poster Presentation Australian Diabetes Society and the Australian Diabetes Educators Association Annual Scientific Meeting 2014
What proportion of diabetes patients are not having renal pathology monitoring? (#371)
BACKGROUND
Diabetes and CKD are independent risk factors for CVD but CV risk is increased when both exist. Control of glycaemia, blood pressure and lipids are all within the scope of skill of GP, subsequent CV events could be prevented. Optimising glycaemic control in diabetes has been shown to reduce microvascular event rates and optimising BGL control in patients with CKD will reduce progress of this preventable microvascular complication.
AIM:
Chronic disease management in primary care competes for GP time. We sought to use pathology laboratory data to benchmark rates of renal monitoring as part of the ACOC.
METHODS:
Private pathology laboratory data for the 2012 calendar year was provided. HbA1c test were cleaned and duplicates removed; - Reports by date, gender, postcode, HbA1c value, eGFR, creatine, microalbumin, albumin creatinine ratios results were provided. We analyse eGFR.
RESULTS :
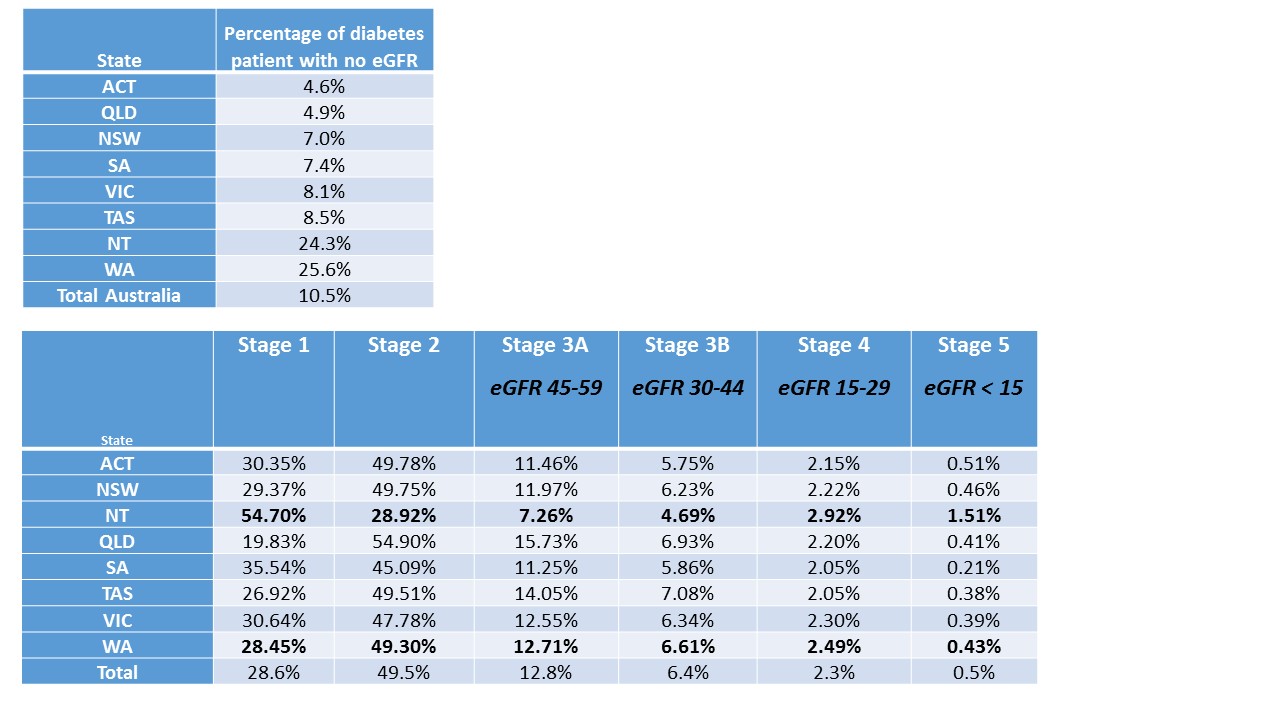
Of 470547 diagnosed diabetes only 421131 had an eGFR/creat recorded, meaning 10.4% (4.64% to 25.57%) did not have renal monitoring. Through geo-epidemiological analysis we identified how each state contributed helping identify where interventions could be directed. Also analysed is CKD stages by state and territory
DISCUSSION and CONCLUSION:
We cannot manage what we don’t measure. The data suggests there is a high percentage of patients with unknown renal status. Lack of monitoring will impact on CV outcomes and decisions for therapy intensification or reduction. Further analysis by postcode and ML is warranted and will allow identification of areas in each state that would benefit from support, education and systems to help GP optimise CV outcomes in patients with diabetes. Queries raised are why there is a dissociation between absent testing and lower CKD rates eg WA and NT