Poster Presentation Australian Diabetes Society and the Australian Diabetes Educators Association Annual Scientific Meeting 2014
Inter-regional differences in the real-world achievement of glycaemic control with dual OAD combinations for the treatment of T2DM (#310)
Guidelines recommend individualisation of care when treating T2DM patients. In real-life, suboptimal glycaemic control is commonplace, despite attempts to optimise therapy intensification based on patient characteristics. EDGE was a 1-year, observational study in T2DM patients, conducted across five world regions. Here, we present a post-hoc analysis of the differences in overall effectiveness and tolerability of any dual oral anti-diabetic drug (OAD) combination, and explore the possible factors affecting treatment success across regions.
Eligible patients were assigned to either the vildagliptin or ‘other OADs’ (excluding incretin therapies) cohort after add-on treatment, prescribed based on clinical judgement, was started. The primary endpoint (PEP) was achievement of an HbA1c reduction of >0.3% without peripheral oedema, hypoglycaemia, discontinuation due to a gastrointestinal event or weight gain ≥5% at 1 year. Secondary endpoint (SEP) included the attainment of HbA1c <7.0% without hypoglycaemia or weight gain ≥3%.
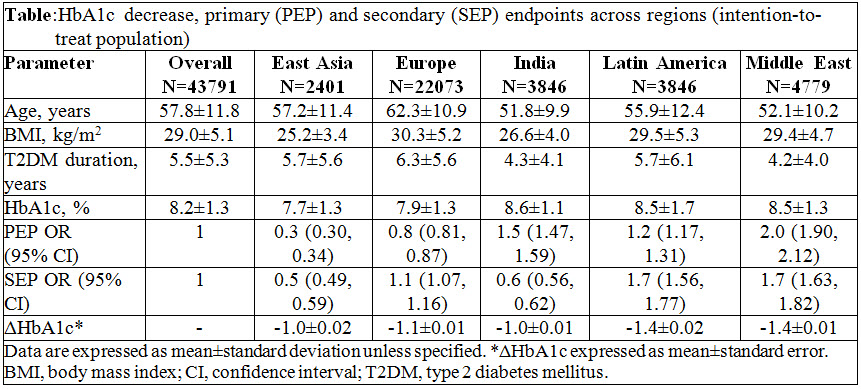
Overall, 45868 patients were enrolled (vildagliptin: 29759; other OADs: 16078; not assigned: 31). The patients’ baseline characteristics varied markedly across regions (table). European patients were ~10 years older with a longer T2DM duration compared with patients in India and Middle East. Patients in Europe, Middle East and Latin America had a higher BMI than patients in India and East Asia. At the time of dual-therapy initiation, HbA1c was better controlled in East Asia and Europe than in other regions. The odds of successfully achieving the PEP were higher in India, Latin America and Middle East compared with other regions (table). The odds of successfully achieving the SEP were highest in Latin America and Middle East despite high baseline HbA1c (table).
EDGE demonstrates lack of glycaemic control across regions, as indicated by high mean HbA1c at treatment intensification. The differences across regions in reaching glycaemic targets without tolerability issues, independent of dual therapy, may be explained by the differences in baseline characteristics, including T2DM duration, access to and intensity of care, lifestyles, genetic variations and pathophysiology of T2DM.